Download this article in magazine layout
Download this article in magazine layout
- Share this article
- Subscribe to our newsletter
One Health – towards a more inclusive science
In 1997, Marcel Tanner, the then director of the Swiss Tropical and Public Health Institute (Swiss TPH) asked me whether, as a veterinarian, I could take a look at the health care of mobile pastoralists (nomadic and transhumant livestock keepers) and their animals in Chad. This mostly nomadic population group falls through the mesh of the Chadian health care system and is completely undersupplied. On this occasion, I remembered my doctoral supervisor Hans Fey, a professor of microbiology at the University of Bern's Faculty of Veterinary Medicine, in Switzerland, who introduced me to the term “One Medicine”. Coined in the 1960s by American epidemiologist Calvin Schwabe, it says that there is no paradigmatic difference between human and veterinary medicine and that both share the same scientific principles.
From “One Medicine” to “One Health”
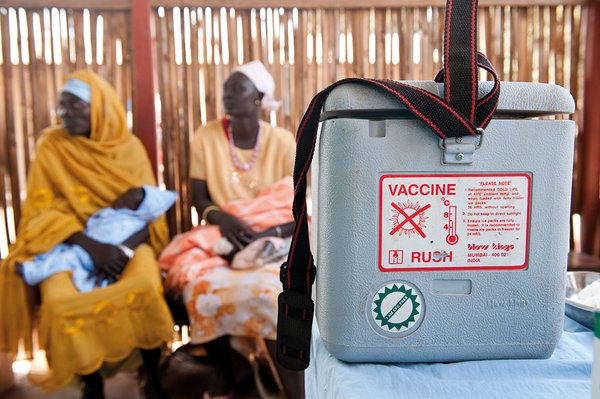
In 1998, as part of a project supported by the Swiss National Science Foundation, an interdisciplinary team of human and veterinary medical staff started to investigate the health of people and their animals on the south-eastern shore of Lake Chad. To our surprise, we found that more animals than children were vaccinated. In a participatory transdisciplinary process with representatives from the population, authorities and science, we agreed on the implementation of common vaccination campaigns for humans and animals. When the veterinarians started organising vaccination campaigns for animals, they took human medical staff with them in the same vehicle. While the vets vaccinated cows, the health workers vaccinated children and women and provided people with medicines and conducted health training, giving a population group previously excluded from care access to health services. The shared use of the cold chain and transport also saved time and money compared to separate services.
This work was the starting point for our theoretical and methodological development from “One Medicine” to “One Health”, with a stronger emphasis on public health and disease prevention. One Health promotes cooperation between representatives from science, authorities and the population. This increased communication helps not only to gain a deeper understanding of the situation, but also to develop better solutions that are supported by all stakeholders and can therefore have a lasting effect. “One Health” therefore means an added value for the health of people and animals and is attractive for health authorities thanks to the financial savings in healing and disease control costs. This is achieved through closer, interdisciplinary and transdisciplinary cooperation on a par between human and veterinary medicine, other natural sciences and the humanities.
Efficient, cost-saving and universally applicable
How can the added value of closer cooperation between human and veterinary medicine be shown? With statistical methods, we can demonstrate that with an interdisciplinary approach, the source of zoonoses (diseases that are transmitted from animals to humans) can be found much more quickly than when humans or animals are examined on their own. Using mathematical models and economic analyses, we see that zoonoses such as brucellosis and rabies can be controlled and eventually eliminated at lesser cost if we contain them in reservoir animals instead of just treating affected people. The joint investigation of schistosomiasis in humans and cows in Côte d’Ivoire showed us a previously neglected high proportion of hybrid forms between animal (Schistosoma bovis) and human (Schistosoma haematobium) parasites in humans. This demonstrates how a zoonosis can develop with unrestricted contact between humans and animals.
One Health approaches are not limited to infectious diseases, but can also be used in many other contexts, for example in rehabilitation therapy. Together with psychologists, we developed and examined animal-assisted therapies for patients with brain injuries, in which the well-being of the animals used is just as important as that of humans. In cooperation with microbiologists, we can show that keeping pets in retirement homes does not lead to a risk of antibiotic-resistant bacterial diseases in humans, but that dogs and cats contribute to human wellbeing. Together with cancer epidemiologists, we investigated the conditions for a joint registration of tumours in humans and dogs. Since dogs often develop tumours more quickly than humans in their lifetime, they could be important in monitoring environmental risks to humans.
Adapting health interventions to local ways of living and thinking
The health of humans and animals is strongly influenced by social, cultural and linguistic factors. If we involve sociologists, anthropologists, linguists and cultural scientists on an equal footing in research planning from the start, we can take these influences into account more precisely. In Guatemala, we managed to enter into a dialogue between Maya healers and biomedically trained doctors. This dialogue showed that the differences between the respective approaches to creating knowledge (epistemologies) were simply too great to form linkages. However, we did recognise the importance of letting patients choose their health care system without forcing them into a conflict of loyalty between different medical systems. In this way, their spiritual, emotional and physical health needs can be better considered at the same time. This dialogue is welcomed by the Maya healers. It is just the beginning, and can be continued with mutual respect.
In northern Mali, a Swiss cultural scientist was able to collect more precise data on the health of Tuareg women than a Malian doctor. This was the case because, apparently, the gender difference represents a greater barrier to communication about health and reproduction than differences in national origin. In the same context, a precise linguistic analysis of word meanings in local languages showed that the loss of knowledge and understanding (epistemicide) can (and must) be prevented through an interest in other ways of thinking and that a common language (lingua franca) should be used carefully.
In rural population groups in Chad, new conceptualisations of “access to health care” and “socially layered resilience” by medical anthropologist Brigit Obrist were groundbreaking in gaining a better systemic understanding of the barriers to the implementation of health interventions. We elaborated these approaches into mixed quantitative-qualitative methods which showed that health interventions in different countries must be adapted to local ways of living and thinking in order to be effective – not the other way around. Generally speaking, these experiences have taught us how a more integrative science creates a gain in knowledge that could not be generated without cooperation.
Involving the population and authorities
In all of our One Health projects, we maintain intensive partnerships with local research institutes and universities in accordance with the guidelines of the Commission for Research Partnerships with Developing Countries (KFPE) of the Swiss Academy of Natural Sciences. The development of health care cannot be limited to the academic field, but must include the population and authorities in the co-production of implementation knowledge. Although many participants in such processes have no formal training, they are nonetheless experts who bring knowledge that is often hidden from purely academic approaches. In this way, in iterative, participatory stakeholder meetings, we can develop effective health care in a very targeted manner which is feasible for the authorities and acceptable to the population (also see articles "Adopting the One Health approach in international practice" and "Towards better livelihoods of livestock-keeping communities").
Moving towards a modern theory of health
Although more integrating and systemic approaches to health have emerged recently, we are observing an accelerated fragmentation of human and veterinary medicine into a growing number of sub-disciplines, which repeatedly leads to misinterpretations. The exponentially growing specialist literature cannot possibly be surveyed by individuals.
At the same time, we are observing, especially using the example of COVID-19, how complex the relationships and dependencies between people, animals and the environment are. How can we move in the direction of a modern theory of health suited to face the new complex challenges of global change? Health must be viewed as the sphere of influence of human actions within human-environment systems or ecosystems approaches to health. We also speak of “health in social-ecological systems” (see Box below).
Health concepts at a glance
One Health is, in the first place, at the intersection of human and animal health, aiming to demonstrate a benefit from a closer cooperation of human and veterinary medicine. Clearly, large sections of separated human and animal health do not require a One Health approach. Broader approaches, considering interactions of health and the environment, within social-ecological systems (SES) comprehend One Health, which is thus embedded within ecosystem approaches to health (EcoHealth), for which a newer term, “Health in Social-Ecological Systems” (HSES), has been coined. SES are most often delimited by a given context of a country or a region. One Health includes social and environmental (ecological) factors, reaching beyond the strict limits of public and animal health.
Planetary Health conceptual thinking aims to identify co-benefits across targets, but remains centred on human health and does not explicitly include animal health. Planetary Health can be seen as a historical extension from global health and international health. It attempts to demonstrate linkages of global environmental change and health, which are hard to prove, based on the inherent data variability, confounding factors, and the duration and scale of the phenomena. We argue that One Health should still be at the centre of interest, building inter-sectoral cooperation from the inside and gradually expanding it to more complex issues and health security hazards across the whole of the SES, as the evidence base for its effectiveness matures.
This perspective includes scaling of systems biology aspects from the molecular and cellular level up to human and animal populations, which helps us understand health explicitly as a consequence of processes in complex human-environment systems. This also includes unpredictable, emergent phenomena (emerging diseases) in the sense of Alfred North Whitehead’s process philosophy. For example determining the origin of the current COVID-19 pandemic to be able to prevent such outbreaks in the future (see Box below).
Why transdisciplinary approaches are needed – the example of COVID-19
The importance of transdisciplinary approaches can be shown well using the example of the COVID-19 outbreak. Epidemiologists and virologists claim the scientific authority to interpret the current pandemic, but not to recommend how society should deal with it. Governments and scientists cannot solve this dilemma on their own. All actors have interests they are pursuing, so a social consensus can best be achieved through a participatory (transdisciplinary) process including representatives of all interest groups.
Most of the Corona viruses have been found in wildlife and livestock. Only few Corona viruses have adapted to humans. Some of the animal viruses in cattle, dogs and humans are genetically close to SARS-CoV-2, the virus causing COVID-19. It is possible that the exposure to animals carrying Corona viruses may elicit a cross-protection against COVID-19 infection and the severity of the clinical course. More research is needed to elucidate possible cross-protection between human and animal Corona viruses.
From a One Health perspective, human, domestic animal and wildlife disease surveillance should be integrated and closely communicated. Integrated surveillance-response systems show that the earlier a zoonotic agent is detected in the environment, in wild animals or domestic animals, and the better the monitoring data for humans, animals and the environment are communicated with each other to prevent an outbreak, the lower the cumulative cost will be. The ongoing COVID-19 pandemic is a striking example in which early detection was missed in wild or domestic animals. There is an urgent need to get to know better the interfaces of the transmission of pathogens between the environment, wild animals, domestic animals and humans as part of a complex human-environmental system (or social-ecological system [SES]).
In order to prevent further pandemic risks through the use of integrated human – animal surveillance-response systems on a global level, we also urgently need to investigate the biosecurity of live animal markets, intensively bred chickens or pigs and other farm animals as well as the risks of transmission between wild and farm animals. To improve biosecurity in live animal markets and on farms, animal welfare needs to be fundamentally changed. Animals are often kept, transported and slaughtered under unacceptable hygienic conditions. At the same time, we must not forget that animal husbandry contributes to the livelihood of hundreds of millions of smallholders. Drastic control measures can lead to loss of income and lead to poverty and hunger. For this reason, all stakeholders (e.g. farmers, traders, butchers, consumers, administrators and scientists) should be involved in developing locally adapted biosecurity and animal welfare measures while maintaining economic activity.
The inescapable relationship between humans and their environment
The “One Health” concept considers the health of people, animals and their environment together and thus transcends people’s traditional anthropocentric perspective. It keeps an eye on the wellbeing of both people and wild and domestic animals in their environment. So it is really about the inescapable relationship between humans and their environment, which includes animals. Such a broader approach is also reflected in the remarkable current initiative to bring animal health and animal welfare to the United Nations by means of a UN convention. This makes it clear that concepts addressing the mutual dependence and influence of humans, animals and the environment, to which One Health belongs, find resonance in a wide variety of academic disciplines such as philosophy, cultural studies, anthropology and law.
Contribution to societal problem solving
Of course, reductionist, basic research is still required at the forefront, especially for the development of new antibiotics or vaccines. But complementary to this, we need more integrating systemic approaches which have the overall social perspective in view and include academic, political and civil actors in finding solutions.
The Organisation for Economic Co-operation and Development (OECD) recently approved a report on the promotion of transdisciplinary research. The report recommends the governments of the member states to use sustainable resources for transdisciplinary research and to involve the public and private sectors in this. Research funding institutions should develop new criteria for the quality of transdisciplinary research and programmes for their funding, while universities should offer modules for training in transdisciplinarity and promote the careers of young women scientists in this field.
Who would have guessed that the study of nomads and their animals that began 23 years ago would open the way to a systemic view with a transdisciplinary approach? Whenever we go down such a path, far-reaching consequences for an inclusive and interwoven science can arise.
Jakob Zinsstag is a veterinary epidemiologist. He is deputy head of the Epidemiology and Public Health department at the Swiss Tropical and Public Health Institute (Swiss TPH), an associated institute of the University of Basel.
Contact: jakob.zinsstag@swisstph.ch
This article is based on a contribution by the author to the bulletin “Lebensräume/Lieux de vie”, 2/20, published by the Swiss Academy of Humanities and Social Sciences (SAHS).
References and further reading:
Bennett, K., 2015. Towards an epistemological monoculture: Mechanisms of epistemicide in European research collaboration., in: (eds.), R.P.A.a.C.P.-L. (Ed.), English as a scientific and research language. de Gruyter Mouton, Boston.
Gandolfi-Decristophoris, P., De Benedetti, A., Petignat, C., Attinger, M., Guillaume, J., Fiebig, L., Hattendorf, J., Cernela, N., Regula, G., Petrini, O., Zinsstag, J., Schelling, E., 2011. Evaluation of pet contact as a risk factor for carriage of multidrug-resistant staphylococci in nursing home residents. Am.J Infect Control.
Hediger, K., Meisser, A., Zinsstag, J., 2019. A One Health Research Framework for Animal-Assisted Interventions. Int J Environ Res Public Health 16.
Lechthaler, F., Abakar, M.F., Schelling, E., Hattendorf, J., Ouedraogo, B., Moto, D.D., Zinsstag, J., 2018. Bottlenecks in the provision of antenatal care: rural settled and mobile pastoralist communities in Chad. Trop Med Int Health 23, 1033-1044.
Mosimann, L., Traore, A., Mauti, S., Lechenne, M., Obrist, B., Veron, R., Hattendorf, J., Zinsstag, J., 2017. A mixed methods approach to assess animal vaccination programmes: The case of rabies control in Bamako, Mali. Acta Trop 165, 203-215.
Münch, A.K., 2012. Nomadic women's health practice: Islamic belief and medical care among Kel Alhafra Tuareg in Mali. Schwabe, Basel, Switzerland.
Obrist, B., Iteba, N., Lengeler, C., Makemba, A., Mshana, C., Nathan, R., Alba, S., Dillip, A., Hetzel, M.W., Mayumana, I., Schulze, A., Mshinda, H., 2007. Access to health care in contexts of livelihood insecurity: a framework for analysis and action, PLoS medicine, pp. 1584-1588.
Obrist, B., Pfeiffer, C., Henley, R., 2010. Multi-layered social resilience: a new approach in mitigation research. Progress in Development Studies 10.
OECD, 2020. Addressing societal challenges using trandisciplinary research, in: publishing, O. (Ed.), OECD Science, Technology and Industry Policy Papers. OECD, Paris, p. 80.
Ostrom, E., 2007. A diagnostic approach going beyond panaceas. Proceedings of the National Academy of Sciences 104, 15181-15187.
Schelling, E., Bechir, M., Ahmed, M.A., Wyss, K., Randolph, T.F., Zinsstag, J., 2007a. Human and animal vaccination delivery to remote nomadic families, Chad. Emerging Infectious Diseases 13, 373-379.
Schelling, E., Wyss, K., Diguimbaye, C., Bechir, M., Taleb, M.O., Bonfoh, B., Tanner, M., Zinsstag, J., 2007b. Toward Integrated and Adapted Health Services for Nomadic Pastoralists and their Animals: A North-South Partnership, in: Hirsch Hadorn, G., Hoffmann-Reim, H., Biber-Klemm, S., Grossenbacher, W., Joye, D., Pohl, C., Wiesmann, U., Zemp, E. (Eds.), Handbook of Transdisciplinary Research. A Proposition by the Swiss Academies of Arts and Sciences. Springer, Heidelberg, pp. 277-291.
Schwabe, C.W., 1984. Veterinary medicine and human health. Williams & Wilkins, Baltimore (USA).
Zinsstag, J., Schelling, E., Waltner-Toews, D., Tanner, M., 2011. From "one medicine" to "one health" and systemic approaches to health and well-being. Prev.vet.med. 101, 148-156.
Zinsstag, J., Schelling, E., Waltner-Toews, D., Whittaker, M., Tanner, M., 2015. One Health: The theory and practice of integrated health approaches. CABI.
Zinsstag, J., Utzinger, J., Probst-Hensch, N., Shan, L., Zhou, X-N., 2020. Towards integrated surveillance-response systems for the prevention of future pandemics. Infectious diseases of poverty. In press.
Video (Youtube): Deep Transdisciplinary Exchange between Maya healers and medical and veterinary scientists in Peten, Guatemala
https://www.youtube.com/watch?v=lfVQnsqLbas&feature=youtu.be
Commission for Research Partnerships with Developing Countries (KFPE): 11 Principles and 7 Questions.
https://naturalsciences.ch/organisations/kfpe/11_principles_7_questions
Global Animal Law Association
www.globalanimallaw.org
«Partnering for change» - Free online course on transdisciplinarity
www.futurelearn.com/courses/partnering-for-change
Schweizerische Akademie der Geistes- und Sozialwissenschaften: One Health: Auf dem Weg zu einer integrierten Wissenschaft:
https://sagw.ch/sagw/angebot/publikationen/details/news/bulletin-220-lebensraeume-lieux-de-vie/