 Download this article in magazine layout
Download this article in magazine layout
- Share this article
- Subscribe to our newsletter
From research to implementation strategies – One Health Capacity Building
One Health has its roots in veterinary medicine, so it is unsurprising that traditional One Health research should focus on zoonotic diseases, which are transmittable between humans and animals. While interdisciplinary collaboration has been at the heart of One Health since its inception, the involved disciplines were initially limited to veterinary and human medicine along with their allied public health disciplines. The original term ‘One Medicine’ indicated that both human and veterinary medicine share a substantial body of knowledge, including physiology and pathology. One Medicine, therefore, called for convergence of medical education and knowledge integration of medical research. Essentially assessing the biological similarities and difference between animals and humans to gain understanding about transmission, emergence and treatment of communicable and non-communicable diseases, research following this traditional approach is primarily in the sphere of comparative medicine. Vaccine development, cancer treatment as well as the use of pig heart valves to treat human cardiovascular disease are among the medical advances evolving from research in comparative medicine. With the formulation of the “12 Manhattan Principles” at the conference of the Wildlife Conservation Society in 2004, the rather clinical One Medicine evolved towards One Health by placing a strong emphasis on the underlying ecological and social factors that determine the health of both animals and humans. Inevitably, this expansion of the approach extended the range of disciplines involved in One Health research, which nonetheless remains dominated by the medical disciplines with a consistent focus on controlling zoonotic diseases via awareness building, vaccination, monitoring, outbreak detection and treatment.
Driving knowledge-building – a look at the global institutional landscape
In the late 2000’s, the institutionalisation of One Health was initiated at global level. In 2007, the One Health Initiative was formed with the sole purpose of promoting One Health. In 2009, the One Health Commission was founded in Washington D.C. with the main mission of raising awareness of One Health among the general public and policy-makers and educating a future One Health workforce. These organisations understood early on that One Health research requires collaboration between disciplines which do not traditionally work together as well as researchers with transdisciplinary skills enabling such collaborative research. Another important body of the One Health landscape is the One Health Platform, a Scientific Reference Network linking scientists of various disciplines and industrial and governmental stakeholders to drive One Health research and integrate knowledge. The One Health Platform has initiated “One Health Day”, celebrated by decentralised events world-wide on the 3rd November to raise awareness of and spread knowledge on One Health. Additionally, it organises the “One Health Congress” and the “One Health Forum”, bringing together interdisciplinary scientists, policy-makers and the private sector to share research results and disseminate evidence-based recommendations.
A great acceleration of One Health research was noted after its endorsement by international organisations. The “Tripartite Agreement” between the World Health Organization (WHO), the World Organization for Animal Health (OIE) and the Food and Agriculture Organization (FAO) was published in 2010. The Agreement set out that these major organisations would collaborate to tackle the complex health challenges arising at the human-animal-environment nexus, as these cannot be solved by any one sector in isolation. Already in 2009, the U.S. Center for Disease Control (CDC) established its One Health Office that is focused on monitoring and controlling emerging and zoonotic infectious diseases by building partnerships across the human, animal and environmental sectors. Additionally, a key priority of the CDC One Health Office is to help countries around the globe to implement One Health. The Zoonotic Disease Prioritization Tool, developed by the CDC, is viewed as an important first step towards enabling the implementation of One Health at national (or regional) levels, as any form of collaboration initially requires a consensus about what challenges need to be jointly tackled.
Focusing on antimicrobial resistance and zoonotic diseases
One Health has become a priority on the global policy agenda, primarily due to the human health risks exhibited by emerging and zoonotic diseases as well as antimicrobial resistance (AMR). These topics are consequently also the topics that are being prioritised for One Health research. In the sphere of AMR, the scientific evidence is quite clear and alarming. Pathogens are getting increasingly resistant, and such resistant pathogens or resistance genes are found in environmental samples across the globe. From a purely scientific standpoint the solutions to the growing problem of AMR are quite simple and straightforward. The usage of antimicrobials needs to be significantly reduced in human and veterinary medicine as well as in agriculture. However, from an interdisciplinary perspective, the issue is more complex. For example, banning antibiotics for livestock has impacts on farmers’ livelihoods and animal welfare. Therefore, regulation is required rather than outright bans. Reducing antibiotic use in human populations calls for significant behaviour change among patients and prescribers, for which education and health promotion campaigns are needed. Also, low-income populations overuse antibiotics more frequently than high-income populations, while at the same time, the increasing accessibility to these drugs in low-income settings is viewed as a huge success of the health system.
In the sphere of emerging and zoonotic diseases, the evidence base is a lot more volatile. While in principle, the mechanisms of zoonotic spill-over are understood, it is highly difficult to predict which pathogen will spill over where and when, and it is even more difficult to predict the disease burden of such pathogens. Consequently, there is a general consensus among One Health scientists that integrated disease monitoring is required. Disease surveillance data of wildlife, livestock and humans need to be integrated into a common platform to allow integrated analysis and subsequent prediction of spill-over hotspots and targeted One Health action.
The knowledge gaps in One Health are increasingly moving out of the medical disciplines and into political science, agricultural science, sociology, economics, data science and geography. A primary question that needs to be addressed is how One Health can be implemented, and what governance structures, institutions and funding mechanisms are required. This is very closely linked to scientifically proving the efficiency and effectiveness of One Health to address the complex health challenges. While it is commonly claimed that One Health interventions are more cost-effective compared to multiple sectoral interventions, very few studies exist which actually provide empirical evidence for this claim. One Health also requires changes in behaviour at both community and economic and political level. To address these knowledge gaps, it is necessary to train and educate an interdisciplinary workforce, looking beyond the classical medical and health science disciplines.
One Health education in the Global North
More and more One Health courses have been introduced world-wide since the high-level endorsement of the WHO, OIE and FAO. In the USA, a number of universities are offering degree courses in One Health. The School of Public Health of the University of Washington, for example, has established the Center for One Health Research, while the University of Arizona and the Midwestern University are offering Master degrees in One Health. Penn State, Texas A&M, Berry College and Ferrum College are running an undergraduate Minor course in One Health. In Europe, the number of such degree programmes is also growing. The London School of Hygiene and Tropical Medicine is offering a Master course on One Health in collaboration with the Royal Veterinary College. The Universities of Liverpool, Edinburgh and Glasgow are running Masters level One Health degree courses. Inside the EU, the University of Utrecht offers a MSc One Health within the Biomedical Science discipline. Université de Tours, Universitat Autònoma de Barcelona and Hannover Medical School are running a Masters programme on Infectious Diseases and One Health, with students studying one semester each in France, Spain and Germany. In cooperation with the Swiss Tropical and Public Health Institute, the University of Basel is offering free online courses on One Health.
At doctoral level, two programmes are being offered in Europe, among them the EU-funded One Health European Joint Programme, which has 37 partner institutions and runs 16 doctoral projects. The only structured programme is the One Health and urban transformation graduate school run at the University of Bonn’s Center for Development Research in cooperation with the University of Applied Science Bonn Rhein Sieg and the United Nations University (see Boxes below).
THE ‘ONE HEALTH AND URBAN TRANSFORMATION’ GRADUATE SCHOOL
The NRW Forschungskolleg ‘One Health and urban transformation’ is a graduate school funded by the state of North Rhine-Westphalia’s Ministry of Culture and Science and is jointly operated by the University Bonn, the University of Applied Science Bonn Rhein-Sieg and the United Nations University – Institute for Environment and Human Security. At the graduate school, 13 doctoral students conduct their research on various One Health topics at the four study locations of Accra (Ghana), Ahmedabad (India), Ruhr Metropolis (Germany) and São Paulo (Brazil). They have diverse academic backgrounds, including public health, geography, biology, mathematics, soil science, sociology and nutritional science. The on-going research projects were developed transdisciplinarily through close collaboration with stakeholders from politics, academia, the private sector and civil society. As a result, interdisciplinary, action-oriented research projects were conducted to holistically examine health challenges of the One Health nexus in the context of urban transformation processes (see next Box). A second batch of doctoral students will begin the structured programme in January 2021.
The first batch of the graduate school doctoral students. Photo: Timo Falkenberg
Identifying barriers to One Health implementation in India
Doctoral student Yasobant Sandul has conducted his research in the context of Ahmedabad, India, aiming to operationalise One Health at municipal level. Sandul examined the current degree of collaboration between human, veterinary and environmental sectors and assessed the barriers to One Health implementation. Understanding the degree of collaboration at the administrative/ policy, provider and community levels serves as an important first step in developing One Health implementation strategies. The extensive research resulted in a five-step process to assess and advance the implementation and operationalisation of One Health, comprising the prioritisation of goals, identification of actors, assessment of current network cohesion, establishment of decision-making processes and identification of enablers and barriers.
In the context of the current research, the focus was on controlling zoonotic diseases, therefore, the One Health Zoonotic Disease Prioritization (OHZDP) tool of the CDC was utilised. The intersectoral stakeholder group prioritised rabies, brucellosis, influenza and Crimean-Congo haemorrhagic fever for collaborative One Health actions. However, the research also found overall low commitment to intersectoral collaboration during non-outbreak periods, which constrains sustainable One Health operationalisation.
More information:
www.zef.de/onehealth.html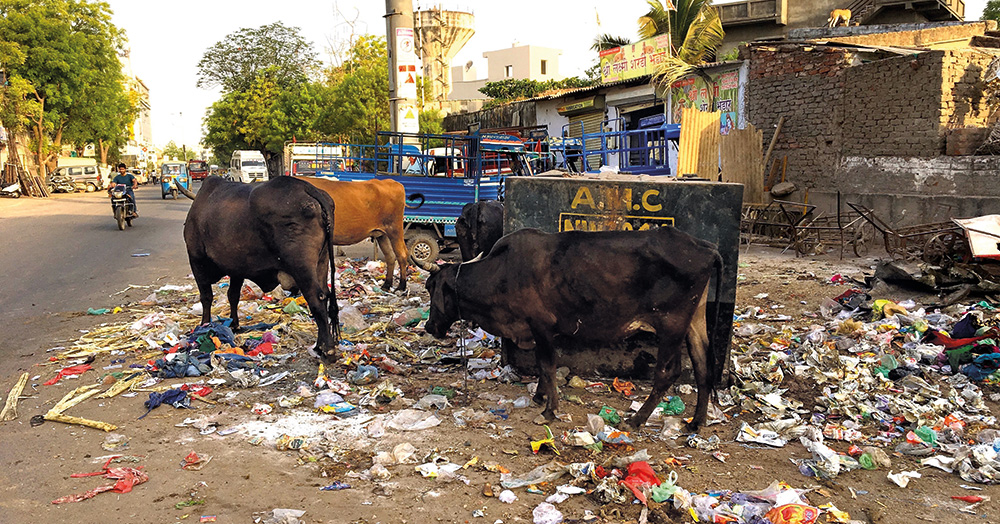
Cows sefting through rubbish for food in Ahmedabad, India. Photo: Timo Falkenberg
One Health capacity building in the Global South
As mentioned above, the CDC is contributing to the implementation of One Health by advising national governments and developing tools for prioritisation. Various international organisations, including the World Bank, WHO and FAO, are facilitating the development of intersectoral collaboration for One Health implementation in Africa and Asia. Governmental and private donors, such as Germany’s Federal Ministry for Economic Cooperation and Development (BMZ), USAID, the Rockefeller Foundation and the Wellcome Trust, are financing One Health capacity building, including training programmes for the health workforce and expansion of transdisciplinary competences. Great achievements have already been attained, as reflected by the Afrique One-ASPIRE Alliance, which is a consortium of research institutions in Chad, Ivory Coast, Ghana, Tanzania, Uganda and Senegal, or the Africa One Health University Network (AFROHUN), which is a network of 16 universities in Cameroon, DR Congo, Ethiopia, Kenya, Uganda, Rwanda, Tanzania and Senegal, having trained 4,500 students since its inauguration in 2010. At national level, various initiatives have come to fruition which drive the application of One Health on the African continent. Examples include the Kenya Zoonotic Disease Unit, the Cameroon Zoonosis Program, the Uganda Zoonotic Disease Coordination Office and the Ghana One Health Technical Working Group.
In Asia, commitment to One Health is also high. This is exemplified by the One Health Network South Asia and the One Health Network South-East Asia. One Health Hubs have been established in Bangladesh, Pakistan, India, Bhutan, Nepal and Sri Lanka, serving as national coordination centres aiming to expand collaboration between governmental sectors to control zoonotic and emerging diseases. Bangladesh has developed a National One Health Strategic Framework and Action Plan, leading to the establishment of the One Health Secretariat. The Southeast Asia One Health University Network (SEAOHUN) is undertaking the One Health Workforce project with USAID, FAO, ILRI and government institution support. This project trains university faculty members to educate the future One Health workforce.
From concept to policy to practice
One Health is moving from concept to practice, focusing on the sphere of zoonotic and emerging diseases. Capacity building programmes primarily focus on developing cooperation between human and veterinary health sectors for monitoring, detection and control of zoonotic outbreaks and training the according workforce. While it is essential to build capacity for controlling zoonotic and emerging diseases, more disciplines and sectors need to be involved in One Health, where research is starting to move beyond the classical One Health topics, going beyond reactively identifying and controlling disease threats, but aiming to understand and tackle the root causes of the increasing zoonotic spill-over risks by looking into land-use changes, environmental degradation, agricultural practices, community behaviour and animal welfare. One Health requires interdisciplinary expertise and political commitment to move from concept to policy and from policy to practice. Capacity building and educational programmes are growing globally, creating the One Health workforce urgently required to effectively control and prevent the health challenges at the human-animal-environment interface.
Timo Falkenberg is a senior researcher at the Center for Development Research (ZEF), Bonn, Germany and coordinator of the Forschungskolleg One Health and Urban Transformation. He is cooperating with the GeoHealth Center of the University Hospital Bonn (UKB) and is an adjunct faculty member at the Indian Institute of Public Health Gandhinagar (IIPH-G).
Contact: falkenberg@uni-bonn.de
Further reading:
Yasobant et al. (2019) Multi-sectoral prioritization of zoonotic diseases: One health perspective from Ahmedabad, India, PLOS ONE 14(7): e0220152.
https://doi.org/10.1371/journal.pone.0220152.





Add a comment
Be the First to Comment